|
This modality is particularly useful in patients with pain refractory to medications, physical therapy, psychotherapy, chiropractic therapy, and other procedural interventions.įactors that do not seem to positively or negatively correlate with SCS therapy include patient age, duration, intensity, and laterality of pain. However, dorsal column stimulation has shown success for many types of neuropathic and radicular pain syndromes. Level A evidence exists for failed back surgery syndrome (post-laminectomy syndrome), peripheral ischemia, peripheral neuropathy, and angina pectoris. Ultimately, SCS requires the patient's active participation in their care and ownership of the responsibilities involved in the continuous management of their pain syndrome.Īpart from social factors, one of the strongest correlations to success is complex regional pain syndrome (CRPS). Additionally, a response to sympathetic nerve block may correlate positively with stimulation therapy. Any implantable device will require adequate follow-up, re-programming, wound management, and sometimes wireless recharging of the device. Numerous patient factors are, at first, seemingly unrelated to patient response to treatment but play a significant role in the likelihood of a positive response to therapy. Many of these are social factors. Often, patient selection is the most challenging aspect of the decision to offer neurostimulation.  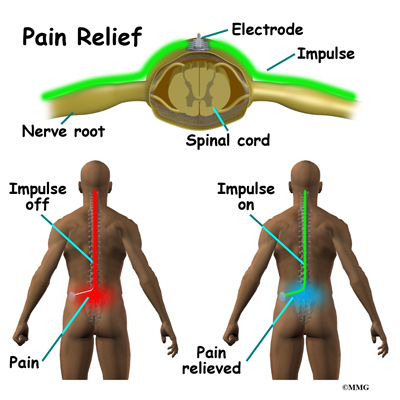
Nociceptive Fibers (peripheral pain receptors) They send this information to second-order neurons located in the spinal cord, mainly in the dorsal horn (central pathways), which are then transmitted via projection neurons to the brainstem (integrative neurons). First, nociceptors receive signals of noxious temperature, chemical, or mechanical stimuli (peripheral neurons). The interrelation between these three systems is responsible for the perceived sensation of pain and the responses associated with it. Multiple pain systems are responsible for the sensation of pain these systems are composed of integrative neuronal sets (conduct excitatory or inhibitory signals on the nociceptors). In other words, stimulation of the touch and vibration nerves “closes the gate” on ascending pain impulses that carry noxious pain stimuli cephalad. This interruption is facilitated by the common nerve synapse location in the substantia gelatinosa of the dorsal horn. In summary, they posed that pain impulses provoked in the periphery, which are carried by C fibers and A-delta fibers, could be interrupted by stimulating larger A-beta fibers. Neurostimulation modalities arose as a response to treating the gate control theory of pain by Melzack and Wall. A similar principle utilizes the central nervous system and the peripheral nervous system stimulation in deep/cortical brain stimulation and peripheral nerve stimulation, respectively. Presently, neuromodulation involves the implantation of leads in the epidural space. 
Initially, this technique applied pulsed energy in the intrathecal space. Spinal cord stimulation uses pulsed electrical energy near the spinal cord to manage pain.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
